by Mrs X.*
*Patient wishes to remain anonymous – Photo modelled from fotalia images
A Personal Account from Menarche to Hysterectomy and beyond
Background
I started my periods at the age of 11 and had few problems with menstruation throughout adulthood. I was prescribed the contraceptive pill at 18, but then stopped at 24 due to a suspected phlebitis in my leg, which my GP advised was a contra indication to using the pill. I took alternative contraception until having my two children, now aged 30 and 33.
I was aware that my mother suffered terribly during her menopause, having symptoms including migraines and depression, though this could have been exacerbated by some stressful personal life events. She started her menopause early at 40, so I was not surprised to start mine relatively early too at 48, when a few minor symptoms began, mostly night sweats affecting sleep and making me tired all the time during the day.
After consultation with my GP, I decided to request the HRT dual hormone pill and found not only did my menopausal symptoms disappear, but also I had a great sense of wellbeing and vitality. Phew! I was now liberated from the draining menopausal symptoms.
Events necessitating the hysterectomy.
In October ’02, aged 51 my husband and I went for a 22 mile bike ride without me feeling any fatigue. However, I had noticed over the preceding months that I needed the toilet at very regular intervals, especially out walking or in the car. The following day I woke up with a pain in my side, rather like indigestion and as the day progressed my breathing became laboured until walking up the stairs was difficult and I couldn’t catch my breath. The next day I saw my GP and he referred me immediately for a chest x ray. I had only just returned home when the surgery rang to tell me to go back to the hospital for investigations and I was admitted onto an admissions ward for 4 days.
Eventually they decided to undertake an ultra sound test where they found I had a tumour on my ovary. This I couldn’t comprehend, as I thought the problem was my lungs which they had to drain fluid off at regular intervals, to enable me to breathe comfortably.
Next thing I knew was a visit from the gynaecologist who informed me that I would need an abdominal hysterectomy! I was a little stunned by the news! He continued to say that he would perform the operation the following week and given that the tumour could be cancerous he would refer me to the cancer specialist nurse who would visit me to give advice and support.
Now I heard the word Cancer, what a big shock, as I had not given the possibility of cancer a thought. They allowed me to return home to prepare for the surgery. That week was an emotional roller-coaster, not only for me, but also my husband and family.
This was my first stay in hospital other than for childbirth and unfortunately my stay on this particular NHS admissions ward was quite traumatic. It was noisy, the food was unappetising, and an older patient who was suffering from dementia attacked me! The whole experience was stressful and given the potential severity of my condition we decided I should take advantage of our medical insurance and arranged to have my surgery in a private hospital.
Preparation for surgery.
I can’t say I focused too much on the negative element of the surgery as I fuelled my energy to make domestic and personal arrangements. We informed my grown up children who no longer lived at home, that I was to have the hysterectomy, but made no mention of the possibility of cancer. I did think of possible outcomes and it even went through my head that I might not need to buy Christmas cards this year!
I collected together and bought nice nightclothes, toiletries, books and magazines etc. a bit like going on holiday. I really wasn’t too worried about the operation as long as I would be better and able to breathe easily. Not been able to breathe properly really caused me a lot of distress and concern.
The hospital stay
This was certainly made a lot more pleasant by admission to a private hospital and a wonderful consultant who gave me a lot of confidence in his abilities. However, because I had been in an NHS hospital, I had to have barrier nursing until swabs had been taken and been proved to be free of infection. I had a private room, en suite bathroom and TV. The food was nutritious and appetising though due to the anaesthetic, I only wanted toast for most of my stay. I still ordered the 3 course dinner, which my husband enjoyed and it negated the need for him to feed himself when he returned home (one less thing for me to worry about!).
On the morning of the operation I had pressure stockings to put on, for which I had been measured and I had to wear these throughout my stay and for a time on my return home to prevent blood clots. These were useful later also for flights abroad!
Thankfully I had shaved already my pubic area, which negated the need for a nurse carrying out this very personal procedure.
I remember being wheeled down to the operating room and meeting the anaesthetist where I requested plenty of anaesthetic as my biggest fear was waking up mid operation and feeling pain, but not being able to tell anyone. He was very reassuring and again he gave me confidence to face the procedure.
Before the surgery they again drained my affected lung and I counted back from 10 to 7 before being knocked out. The next thing I remember was waking up in a very pleasant post- op room. I had no pain as they had given me an epidural delivering morphine and for a couple of days this remained in my arm. I was made very comfortable with loads of cards and flowers arriving by the hour. Indeed, I was overwhelmed by the response from family, friends and colleagues- I felt very loved and valued.
Post op recovery
Once the epidural was removed I had more problems, not particularly with pain- as long as I moved slowly the pain killers were fine. The problems occurred due to the aftermath of the anaesthetic -nausea and constipation – and indeed I was not allowed home until all functions were working properly again. This took about 5 days. I was encouraged to walk about and was weighed every day. As someone constantly watching my weight, I was thrilled to find that I had lost over a stone obviously a combination of womb, tumour and only eating toast for a few days!
Given I had abdominal surgery with a vertical incision just below my panty line I was encouraged to do deep breathing exercises and to start gentle pelvic floor exercises. As a side issue, I have continued to do these on a regular basis and continue them in my yoga class. I am pleased to report that I have not had any urinary complications since the surgery.
Throughout this time my consultant visited daily and he told me that he had removed a tumour as big as a water jug (like the one on my table!) He didn’t know whether it was malignant but it had been sent to the lab for testing. It would be a couple of weeks before I knew the outcome. In the meantime the cancer nurse would make contact with me again.
As I have said earlier I did not feel like eating, but I was encouraged to drink plenty of water. Passing urine the first few days was via my catheter tube, which the nurses monitored all the time. On the third day I had it removed and once I had passed urine normally I did not have any further issues in this department.
Home again – the recovery.
Once home I was informed that recuperation would last for about 3 months, and was given a six-week outpatient appointment to see my consultant again. I was advised to take things easy; no lifting, vacuuming (what a shame) and no driving as a sudden jolt could tear the stitches. Well wishes continued to flood in and my husband took me out for little run outs in the car to break the monotony. Co-incidentally he too had had a minor operation and he was off work with me.
After about 10 days I received a phone call from my consultant- I remember this so well, my husband and I were still in bed early in the morning and as my husband passed the phone to me, my heart started pounding and I did feel scared. However it was good news. The tumour had been a very rare tetroid or monster tumour called a struma ovaria and could have been growing from childhood.
It is a tumour of the ovary composed almost entirely of thyroid tissue with large follicles containing abundant colloid. 5-10 percent become malignant and mine was benign, what a relief and sheer elation. My next phone call was to my cancer nurse to tell her the news and in the nicest possible way said I hoped I would not need to see her again!
Six week check
By this time my scar was healing well and I was able to resume driving. My husband and I decided to join the local Leisure Club and we went swimming most days, followed by some pampering in the spa. I was feeling very fit and well and my consultant was pleased with my progress. He agreed with me using HRT again, but now I would only need the single dose Premarin, which is produced from mare’s urine and he thought would be the safest. Normally one would take a daily tablet, but I quickly found I only needed 3 a week to keep menopausal symptoms at bay.- As my GP regards my medical history as low risk she has allowed me to keep on this dose for the last 12 years.
Life after a hysterectomy.
I returned back to work earlier than expected at 9 weeks and I can honestly say I have never felt fitter now at 63 and retired. I have managed to keep my weight down by healthy eating and regular exercise- yoga, swimming, Zumba, walking, gardening and bike riding. I was not affected psychologically by the hysterectomy, as I had finished child bearing and my reproductive system was redundant.
I was elated I was now fit and indeed no longer at risk of ovarian or cervical cancer and no more cervical smears! I have been able to reassure friends who have needed a hysterectomy of my positive experience and actually my memories of the time now are more of the affection I received, the pampering and the lovely post op time of recuperation and feeling so well.
Post Script – by Lynn Basford
The personal experience of this woman’s story (who wished to remain anonymous), is of course unique to her. The sudden onset of her deteriorating condition meant her preparation period prior to surgery was limited. Nevertheless, there are some revealing insights as how she used positive coping mechanisms that are useful to share, and indeed relate to some areas of our hysterectomy preparation tips.
Chiefly, her attitude was positive, in that she did not dwell too much on the negative, but more about channelling her energy into the preparation that she needed to do, namely: “Domestic and personal issues” as time was not on her side. As we have mentioned earlier, a positive attitude has been shown through various research studies to be of immense benefit to your overall health and well being, and speedy surgical recovery.
Part of her concern was preparing the family and her need requirements during her hospital stay. She bought in new toiletries/books/magazines etc. treating the episode as if she was going on holiday. (A treat for her). Fleetingly, thinking of her own mortality, she mentally thought she would not need to buy christmas cards that year!! How interesting is the world of our minds when under pressure?
After her emergency hospital experience , the noise levels, the poor quality of food and the fact that she was attacked by another patient, she decided (after consultation with her husband and medical team), to make use of her health insurance that enabled her to have private hospital treatment. Such a step made her relax a little about entering a ward environment that was relatively strange for her.
Noise in hospital wards can be a problem, so it may be advisable to take in ear plugs.
Further, she built up a rapport with her consultant, the anaesthetist and cancer specialist nurse, who all gave her confidence in their expertise enabling her to relax.
Part of her preparation and post surgical regime was to undertake breathing exercises , given that this was the primary presenting symptom, and one that continued to raise her concerns. ( NB. it is probable that the fluid that was needed to be drained off her lungs, as she proclaimed , was due to a condition known as abdominal ascites ). As the name indicates there is excess fluid within the abdominal area that eventually pushes up on the lungs and creates difficulty in breathing. Post surgery, this was never an issue, so the underlying problem was clearly the tumour.
During her stay in hospital she was also advised to do pelvic floor exercises and continued these exercises post surgery through to the present day. Enhanced through her personal yoga practice and various sporting activities, such as walking and cycling. By her own admission she did not have any post surgical problems with urinary department , nor with her breathing.
Even though her tumour, whilst benign, was very large and would have been compressing some key internal organs, such as bladder, large bowel etc, her recovery from surgery was relatively uneventful with no obvious co morbid situations. She was, of course, given appropriate levels of analgesics, that would have enabled her to breathe and move around more easily. (However, it is questionable if she would have had the analgesics through an epidural once surgery had been completed, but possibly via an intravenous system).
Mrs X clearly had support from her husband, family and friends, making her feel very loved. A factor that helped her emotional wellbeing. (if we are emotionally well it affects our physical wellbeing as well, or indeed, vice versa). By her own admission she has never looked back from having her hysterectomy and feels fitter now that when she was younger.
Of particular note, she has continued with an exercise regime, including pelvic floor exercises, has had continued loving support from her husband, and has an understanding GP who has identified her risk aspect when prescribing hormonal replacement therapy.
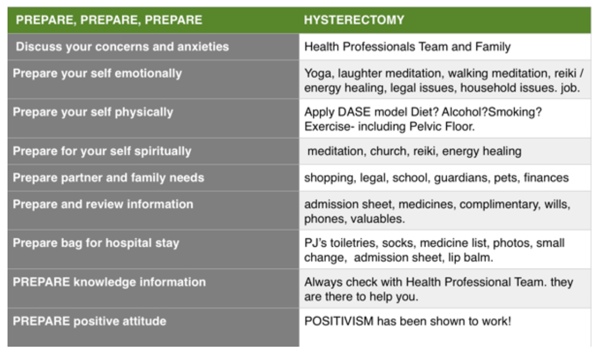
Just to recap, your recovery from surgery can be greatly improved if you consider, and undertake the preparation that the time will allow you and that is appropriate for you. Review table below for aspects of Preparation techniques:
Click on the links below to access all our hysterectomy related articles:
Arm 2: Exercise – Pelvic Floor
Walking in Sunshine – Tips to Prepare for Surgery
Laughter Yoga – What’s the joke?
Arm 5: Medicines & Supplements
Arm 7: Personal & Family Arrangements
Surgical Innovation: Robotic Surgery
Patient Perspective: Experiencing a robotic surgery
Patient Perspective: Experiencing an abdominal hysterectomy
Recovering from Hysterectomy
Recovering from Hysterectomy – The Big Picture
Recovering from Hysterectomy – First 24 hours

