by Professor Lynn Basford
Fear of anaesthesia
One of the most talked about aspects of any surgery is your potential reaction to the anaesthetic. The fear factor is very real, as are the questions that will run through your mind regarding the anaesthetic such as:
- What if I do not wake up?
- Will I feel the surgeon as he/she is performing the surgery?
- Will I hear the team talking?
- Will I feel pain?
- How will I breathe?
And the list continues…
 These feelings are normal, but you should remember that the sophistication of anaesthetics have come a long, long way since the beginnings of Barber Shop Surgery, where anaesthesia was drinking a bottle of spirit, or two and, if you were lucky, some opium!
These feelings are normal, but you should remember that the sophistication of anaesthetics have come a long, long way since the beginnings of Barber Shop Surgery, where anaesthesia was drinking a bottle of spirit, or two and, if you were lucky, some opium!
From a European perspective modern day anaesthesia is dubiously credited to WT Green-Morton ( 1846) 1 who was an American dentist who used ether as an anaesthetic medium. Back in the late 1700’s Sir Humphrey Davy, an Englishman, was experimenting with Nitric Oxide (laughing gas) and Chlorine.2
However, if you go back through the annals of history you will find that in each ancient culture there is evidence that the pursuit of rendering someone unconscious was undertaken for the purpose of healing.
The art and science of anaesthesia has clearly evolved through which surgical intervention can be safely undertaken while the patient is under the watchful, and expert eye of an anaesthetic consultant.
Anaesthetic Assessment
Prior to surgery you will expect to undertake a detailed assessment to ensure any potential risks are accounted for and addressed to ensure your utmost safety. Such a procedure has been fine tuned over the centuries where risks have been greatly minimised and the after effects from anaesthesia reduced.
Today there are more that 55,000 women in the UK annually who have Hysterectomy operations. 3 While in the USA, there are more than 600.000.4
For the most part the assessment will consider your physical and mental health status and may include:
- psychological assessment (fear of dying, being probed with needles, fear of vomiting, or fear of being smothered with anaesthetic mask),
- cardio vascular assessment (hypertension, hypotension, circulatory problems, coronary artery disease),
- respiratory assessment (including smoking history and occupations, asthma, COPD, bronchitis, emphysema, seasonal or food and medication allergies),
- hormonal imbalances, (such as Diabetes Mellitus, thyroid, adrenal, or pituitary dysfunction),
- weight issues – particularly obesity,
- medication history (including illegal drugs, St Johns Wort or Ma Huang, and over the counter drugs),
- Musculoskeletal system (Muscle cramps, osteoporosis, arthritis, metallic hardware, lower back pain, and mobility issues),
- gastro intestinal issues (Hiatus hernia, peptic ulcer, reflux, heart burn, oesophageal problems),
- Liver or kidney problems.
So you can see, there will be no stone unturned prior to the surgery. Every eventuality and potential complications will be fully addressed to ensure your safety and speedy recovery.
Types of Anaesthesia
Depending on the type of hysterectomy and reasons for it, there are two modes through which anaesthesia is carried out:
(i) General Anaesthetic or
(ii) Spinal/Epidural.
1. General anaesthetic
General anaesthetic is more frequently used and enables the anaesthetist to render you unconscious so you feel no pain and are totally relaxed, and he/she can control your breathing and monitor your vital signs through every stage of the proceedings.
To suggest that there are no risks with a general anaesthetic would be unfounded, but the risks are minimised through using a full assessment analysis of your personal situation as indicated above.
NB: The great benefit of having a general anaesthesia is that you sleep throughout the whole surgical procedure and awaken in the warmth of the recovery room.
SHOULD YOU NEED FURTHER INFORMATION PLEASE DISCUSS WITH YOUR TEAM.
2. Spinal/Epidural
Spinal/Epidural is more commonly used for simply hysterectomies that would only take a maximum of couple of hours to perform. With Spinal/Epidural method you are temporarily paralysed from the waist down and moderately sedated.
NB:The benefits of having a Spinal/Epidural is that you a fully awake throughout the whole procedure thus maintaining your refluxes/cognitive responses. In addition, analgesic dosing can occur throughout the whole procedure and recovery time is minimal.
There are however, some known side effects that may include; reaction to the local anaesthetic, injury and infection.
NB: The mode of anaesthesia will be fully discussed with you and your consent given prior to surgery.
What’s next?
So you have been fully assessed, prepared having had your pre op medication and you are wondering what to expect next?
- You will be assigned a nurse and porter who will escort you to the ante room of the theatre. (In some hospitals theatre staff will agrees to play your favourite relaxing music during the procedure. If that is the case in your area remember to bring the music with you).
- Your anaesthetist will greet you along with the theatre staff who will transfer responsibility of your care from the escorting staff. Your name and tag will be checked against your notes to ensure they have the right person. Once established, the proceedings will begin with your anaesthesia depending on chosen method.
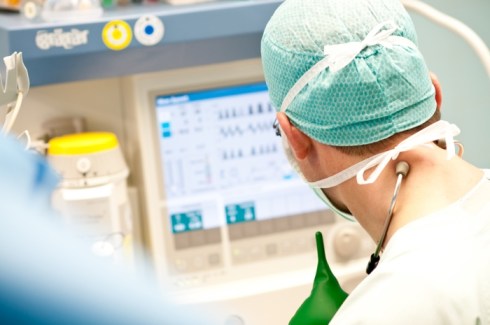
- The anaesthetist will usually insert an IV infusion through which anaesthetic drugs will be administered. Be reassured you will be monitored throughout, including your breathing, your pulse and heart rate and your temperature. In addition, great attention to your privacy and dignity will be upheld by everyone.
- If you are having a spinal block the anaesthetic solution will be injected into the subarachnoid space (subarachnoid block SAB). Your response to this will be determined through pinpricking/coolness. With respect of an epidural anaesthesia the anaesthetic is directed into the spine through a cannula into the epidural space.
- Once assured you are suitably anaesthetised you will be transferred to the main theatre were the surgical team will begin the hysterectomy.
- Your surgeon will insert a catheter into your bladder to decompress the bladder in size and reduce any risk of accidental injury (remember the uterus and bladder are in close proximity to each other). In addition, a bladder catheter makes it easier to monitor urinary output which should normally be 0.5 to 1 ml/kg/hr, and to detect any blood in the urine.
- On completion of your hysterectomy (through whatever means ) you will be transported back to the recover room. Here your care will be transferred to the recovery team who are specially trained to care for all your needs. They will be given detailed information of the total procedure , including findings during surgery, drugs given, your vital sign trends, etc.
- You will be visited by the surgical consultant and your anaesthetist to determine your recovery and post operative responses. If awake, your surgeon will describe what he found and what was needed to be done.
- Once the recovery team are satisfied they will transfer you back under the care of the ward team.
Recovery Room
Here you will wake up but you will still be very groggy and you will be on oxygen until you are ready to leave recovery to go back to the word.
Some people can be nauseous after anaesthetic and this is why it is advisable not to eat or drink for a while. In the recovery room the team will moisten your lips and mouth but will not allow enough fluid that could cause you to swallow as this could trigger nausea.
While in recovery you may be aware of what is going on but you will generally drift in an out of sleep and you may not remember any or all of your time in recovery.
Post Anaesthetic
Anaesthetic affects everyone differently. It will also depend on the length of your surgery as the longer you are under the more you are exposed to the anaesthetic drugs. As you recover from anaesthetic, you may not have any after effects at all but some people may experience some of the following:
- nausea and vomiting
- confusion, brain fog and poor memory (this will pass!)
- a chemical odour from your body and in your urine
- blurred vision
- dizziness
- weakness
- bad dreams, nightmares and anxiety
- feeling tearful
Once you are allowed to eat and drink, eat lightly and drink plenty of water to flush the drugs out of your system. It can take up to a month to really get over the full effects of a long surgery so don’t worry if you feel that your mind is slower than usual, it will get back to normal.
References
1.Wikipedia Encyclopedia ( 10-July 2014), WTGreen- Morton (1819-1868)
2.Wikipedia Encyclopaedia (10- July 2014), Sir Humphrey Davy ( 1778-1829)
3.Hysterectomy Association ( 2014), Supporting hysterectomy through choice and information. http://www.Hysterectomy association.org.uk
4. National Women’s Health Network ( 2014) ,A voice for women a Network for change. http://www.nwhn.org/hysterectomy.
Arm 2: Exercise – Pelvic Floor
Walking in Sunshine – Tips to Prepare for Surgery
Laughter Yoga – What’s the joke?
Arm 5: Medicines & Supplements
Arm 7: Personal & Family Arrangements
Surgical Innovation: Robotic Surgery
Patient Perspective: Experiencing a robotic surgery
Patient Perspective: Experiencing an abdominal hysterectomy
Recovering from Hysterectomy
Recovering from Hysterectomy – The Big Picture
Recovering from Hysterectomy – First 24 hours

